Studies from leading medical centers and even state pharmaceutical quality departments prove that psychoactive substance therapy is more effective than traditional methods of treating mental disorders. It is likely that the demand for such a methodology may become more popular in Ukraine, where psychological problems have increased significantly due to the war. Zaborona attended a conference on psychedelic therapy, where talked to an American veteran who cured PTSD with MDMA and therapists and asked them about psychedelic treatment: how it works, whether it is legal, and whether it is safe.
How does psychedelic-assisted therapy treat mental illness? Here is the experience of a US Marine Corps veteran
Jonathan Lubecky is an American military man who served in the US Marine Corps for four years and another year in Iraq. Jonathan’s contract was signed for 2005-2006, the period when the military operations were most active. Due to the density of shelling, the Balad air base near Baghdad, where Lubecky was stationed, was nicknamed Death Valley in the media.

Jonathan Lubecky in Kyiv, December 6, 2022. Photo: jonathanlubecky / Instagram
Lubecky has been in the combat zone many times: once a sabotage group managed to break through American positions and shoot several soldiers, and in April 2006 a shell hit the building of the toilet where Lubecky was staying. He was unharmed by the debris, but the blast wave left him with a concussion and a brain injury.
After returning from the war, Jonathan suffered a personal tragedy at home: his wife left him, taking his belongings, motorcycle and dog.
Lubecky started drinking. On Christmas Eve, he was sitting in a bar when he heard church bells. He followed the sound and tried to enter the church, but the ministers wouldn’t let him in and told him to come back in the morning. Jonathan broke down in tears and wandered to the war memorial in the city center, where he caught himself thinking about suicide. It scared him, so he went to a military hospital.
The doctors asked him if he had any weapons and ammunition. Jonathan admitted that he had a lot of weapons. Then the hospital gave him six Xanax pills and advised him not to take them all at once. He was told to give the weapons to a neighbor and come back after the holidays. Lubecky came home, drank a bottle of vodka, loaded the gun and pulled the trigger. There was not enough powder in the cartridge, so the bullet did not go all the way into the barrel.
This was the first of five suicide attempts by Lubecky. After the failed suicides, he visited psychotherapists and psychiatrists, who prescribed him antidepressants and worked with him on several psychotherapy methods, but, according to the man, he did not feel much progress.
A few years later, Jonathan enrolled in the North Carolina Military College “The Citadel” to study law and later lobby for the protection of veterans’ rights. At one of the college’s educational events, he met Republican Senator Rand Paul of Kentucky. When he saw Jonathan’s wrists wrapped in bandages, he took the veteran aside: “If you ever feel that way again, I want you to call this number.” Jonathan called a few days later.
So thanks to Paul’s connections, he returned to treatment. The intern who was conducting Lubecky’s psychotherapy session read his file and medical history several times and then handed him a folded piece of paper and told him to open it when he left the hospital. Lubeсki opened the sheet and read, “Google MDMA for PTSD.”
On May 4 of this year, Lubecky tells his story to the public from the stage of a Kyiv conference on psychedelic-assisted therapy. He looks like a happy and satisfied person – which is in stark contrast to his story. Jonathan attended his last session of psychedelic-assisted therapy in 2015. A year later, doctors noted the almost complete disappearance of PTSD symptoms and a significant decrease in depression.

Jonathan Lubecky during his first session of psychedelic-assisted therapy, November 22, 2014. Photo: jonathanlubecky / Instagram
What is psychedelic-assisted therapy (PAT)?
It is a psychotherapeutic practice that uses psychoactive substances, such as MDMA, lysergic acid (LSD), psilocybin, or ketamine.
The therapy has a clear structure:
As a rule, psychedelic therapy lasts from 1 to 6 sessions – the duration of the course depends on the type of disorder and its complexity.

Vladyslav Matrenytskyi. Photo: Ivan Chernichkin / Zaborona
“PAT mainly works with resistant conditions – cases where the treatment of PTSD, depression or anxiety with the available means of psychotherapy or psychiatry, i.e. pharmacology or psychotherapy, is insufficient,” Vladyslav Matrenytskyi, a psychotherapist and founder of the only ketamine therapy clinic in Eastern Europe, tells Zaborona.
Due to the experimental nature of the methodology, official state institutions do not practice PAT. Only private clinics do this. In addition to private clinics, psychedelic therapy is practiced by private psychotherapists.
Currently, there is no legal provision in Ukraine that would regulate this type of therapy. Doctors practicing PAT are actually doing it illegally. However, there are exceptions: ketamine and ibogaine are hardly regulated by law, so anyone can buy them.

Oleh Orlov. Photo: Oleg Orlov / Facebook
“Personally, I am against [private therapists performing PAT],” Oleh Orlov, a scientist and co-founder of the Ukrainian Psychedelic Research Association (UPRA), explains to Zaborona. “We don’t know the quality of the drugs, who works with the patient, what patients are told [during therapy]. This culture [of therapy] is less developed in Ukraine, but we see signs that due to the high demand, people will look for it – and find it. It is possible that due to low-quality specialists, this will be a negative experience.”
Does it work at all?
According to patient feedback and research, yes.
At present, it is impossible to conduct a study of the effectiveness of PAT in Ukraine, as there is no provision that would regulate the therapy and thus determine the legitimacy of such tests. However, in many UN countries, such clinical trials have already been conducted under state control and have determined PAT to be effective. For example, the US Food and Drug Administration has granted psychedelic therapy “breakthrough” status, which accelerates research on psychedelics that show greater efficacy and legitimizes the PAT methodology among society and the government.
The effectiveness of PAT has been proven by many scientific studies. For example, French scientists have found that symptoms of depression, alcohol or tobacco addiction, and obsessive-compulsive disorder decrease after the first psilocybin therapy session. And in this scientific article, researchers from the United States proved the effectiveness of therapy with LSD and MDMA in patients with anxiety disorder, PTSD, and even anxiety among adults with autism.
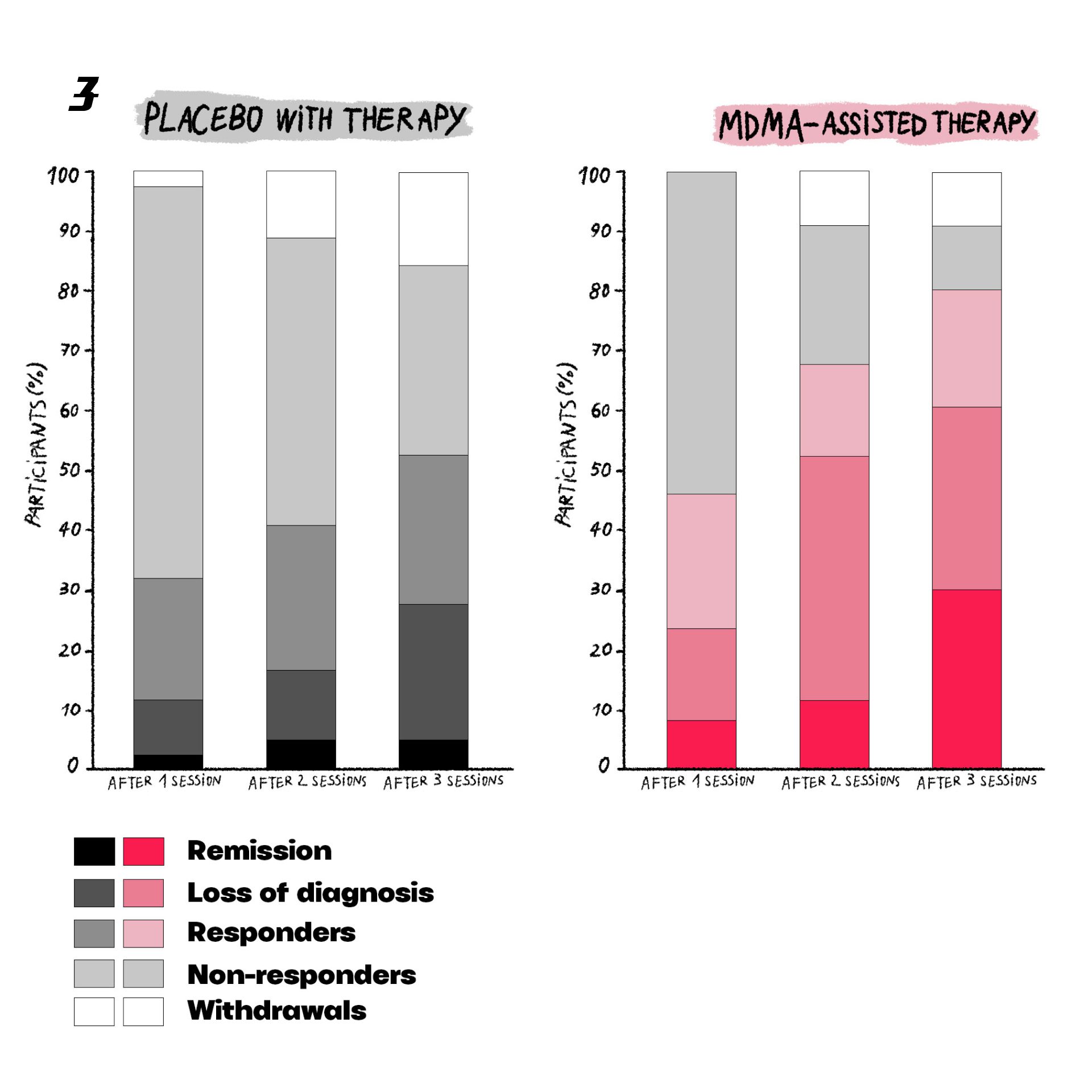
In an American study published in 2021, 88% of patients with PTSD experienced symptom relief after three sessions with MDMA. 67% of them reported a complete recovery. At the same time, the same psychotherapists conducted traditional treatment (without the use of psychedelics) with another group of patients. Of the second group, only 32% of the recipients reported an improvement in symptoms.

Infographic: Maria Petrova / Zaborona. Data: PubMed
“There are many randomized controlled clinical trials under the supervision of the US Food and Drug Administration,” explains Orlov, “This authority has very high requirements for the quality of research, and even the protocols of the studies themselves were developed in close cooperation with the FDA. They put forward certain requirements for scientists, and if they comply with these requirements in terms of data collection, information storage, and the scientific part, only then they allow the study to be conducted. It makes sense to trust them.”
How does assisted therapy differ from using psychedelics at home?
Almost in everything.
Psychedelic-assisted therapy is a process fully controlled by a specialist, and the drugs he uses in practice are of better quality than those purchased from drug couriers.
“You can’t be sure that what you got somewhere is what you wanted to buy,” adds Oleh Orlov, “You need laboratory tests, and it’s problematic to demand them in the black market. If you can’t control the quality, you have nowhere to complain.”
The second difference is that it is illegal to buy and store psychedelic substances at home (the realization that you are breaking the law can negatively affect the psychological state during a psychedelic session). However, the use of such substances is not subject to criminal liability, so you are not violating anything when you see a psychotherapist.
It is mentally difficult to use psychedelic substances for recreational purposes on your own, because
“It’s like comparing anesthesia in a hospital before surgery and injecting anesthesia yourself. What’s the difference? You won’t be able to do all the necessary manipulations at home,” says Orlov.
What does a PAT session look like?
The process can be divided into three conditional phases: preparation, taking psychedelics, and the so-called integration, which is a discussion of the psychedelic experience with a specialist and its implementation.
“The standard protocol usually includes several sessions to diagnose, identify contraindications, and prepare a person. This is followed by one or more sessions of [psychedelic] experience. A session can last 6-8 hours,” says Orlov. “The role of the therapist is not so active: the main idea is not to encourage or guide the person, but to accompany them. If the patient is stuck in introspection, you can help a little bit.”
Orlov adds that PAT’s methodology borrows from standard diagnostic procedures, and the type of therapy used during a patient’s psychedelic experience also belongs to traditional areas-for example, PAT uses the techniques of cognitive behavioral therapy or Gestalt therapy.
Before starting therapy, a patient should undergo a medical examination for contraindications, which a doctor must prescribe. At the preparation stage, the psychotherapist discusses possible side effects and risks with the client and advises on how the process will go. The patient and the therapists also examine the main requests and mental attitudes they will work with.
The dosage of the drug is selected personally by the therapist. If the prescribed dosage is not enough, the patient can take an additional portion in two hours, which will be half of the previous one.
“MDMA acts on the prefrontal cortex and hippocampus: it temporarily reduces reactions to negative emotional memories and increases reactions to positive memories,” says Orlov. “It becomes easier for a person to work with traumatic memory. If we are talking about psilocybin, it turns on a filter in the brain that is responsible for redirecting information. Temporarily, everything starts to be connected to everything, and this allows you to draw new conclusions [about traumatic experiences].”
The session should be held in a specially equipped room with comfortable and safe conditions for the patient. During the session, the client can sit or lie down, and sometimes the therapist may suggest wearing a sleep mask and headphones with selected music.

Collage: Maria Petrova / Zaborona
Some methods still don’t look safe enough. Can PAT do harm?
According to the therapists themselves, both yes (without assistance) and no (reliving negative experiences is part of treatment).
The logical questions related to PAT are as follows: is re-traumatization or fixation on negative experiences possible, which are exacerbated by the effects of psychedelics? And is a so-called bad trip possible?
Oleh Orlov says that there is no such thing as a bad trip in the PAT vocabulary because any reaction will be useful. If a person is faced with traumatic memories, they should not be suppressed. A psychotherapist should help process this experience. The therapist’s role in the process is to listen and guide the patient. He or she can ask questions, but cannot force the patient to talk or think about any specific events. MDMA unlocks hidden feelings and emotions, so it is not uncommon for patients to cry or get angry during these sessions.
“Theoretically, PAT can only additionally traumatize a person if it is performed incorrectly. I know of cases when a person was simply given the drug and told ‘it will help’. The person has used it, they say: “integrate [the psychedelic experience into the treatment process],” and it is not clear how. But in a clinical setting, there are no such cases,” the scientist explains.
Psychedelic-assisted therapy has standard side effects. As a psychostimulant, MDMA increases blood pressure or can cause muscle spasms. However, these symptoms only persist while the substance is still active.
“In theory, psychological dependence [on the drug] can occur if it is used incorrectly. For example, if a patient does not go to a session as a therapy, but tries to simply change their state of consciousness. But this is a dependence not on the drug itself, but on behavioral strategies,” the scientist explains.
Is there a chance that PAT will be legalized in Ukraine in the near future?
It’s hard to predict.
Since the beginning of the full-scale war in Ukraine, the level of mental disorders has increased significantly. According to the WHO, as of the end of 2022, more than 10 million Ukrainians were at risk – the most common mental disorders are PTSD, depression and anxiety disorder. Therefore, an increase in the popularity of the culture of psychotherapy, its demarginalization, and the search for alternative methods in the future is a likely scenario.
On the other hand, given the conservatism of a significant number of parliamentarians and government officials, the process may take years, as is the case, for example, with the legalization of medical cannabis.
“We have enough competent specialists who need to undergo a short training,” explains Orlov, “We are engaging foreign colleagues from around the world who are researching the PAT and are ready to help us implement it in Ukraine. The Ministry of Health says they are open to discussion, and it is important to them that the methodology is scientifically sound. But this process also involves the police and [drug] trafficking control — they have a more conservative position.”